Traditionally, from a payment perspective, healthcare providers have been following a fee-for-service (FFS) model under which the payment was made for each individual service they performed, rather than being paid a lump sum for treating a specific illness or condition.
Under this model, providers were paid for each office visit, procedure, test, or treatment, regardless of the outcome. This model has been the dominant healthcare payment method in many countries.
However, this traditional FFS model has been criticized for incentivizing volume over value, leading to overutilization, inefficiency, and higher healthcare costs.
As a result, alternative payment models, such as value-based care and bundled payments, have been gaining traction in recent years. These models aim to shift the focus from the volume of services provided to the quality of care and outcomes achieved, in an effort to improve the overall efficiency and cost-effectiveness of the healthcare system.
Let’s understand value-based healthcare, its benefits, challenges and how it works.
What is Value-Based Healthcare?
Value-based care is a healthcare delivery model that prioritizes providing quality care to patients while controlling costs. The main idea behind value-based care is to shift the focus from volume-based care, where healthcare providers are paid for the number of services they provide, to value-based care, where they are paid for the outcomes they achieve for their patients.
Value-based care prioritizes patient outcomes, such as improved health, reduced hospitalizations, and improved patient satisfaction, over the number of procedures or tests performed. This model of care encourages healthcare providers to work together and coordinate care for their patients, leading to a more efficient and effective delivery of care.
How Does Value-Based Healthcare Work?
Let’s understand how value-based healthcare works through a patient-centered medical home (PCMH) model.
In a PCMH model, a primary care practice provides comprehensive and coordinated care to their patients. The practice is incentivized to keep their patients healthy and out of the hospital, which helps to control costs and improve patient outcomes.
For example, a patient with diabetes may receive care from a PCMH. The primary care provider in the PCMH would work with the patient to develop a care plan that includes regular check-ins, monitoring of blood sugar levels, and lifestyle changes to manage the diabetes. The provider may also coordinate care with other specialists, such as an endocrinologist or dietitian, to ensure that the patient receives comprehensive and coordinated care.
In this model, the PCMH is paid based on the value of care they deliver, rather than the volume of services provided. For example, the PCMH may be paid a set amount for each patient with diabetes they care for, and they are held accountable for both the cost and quality of care they deliver. The PCMH is incentivized to keep their patients healthy, reduce hospitalizations, and improve patient satisfaction, which helps to control costs and improve patient outcomes.
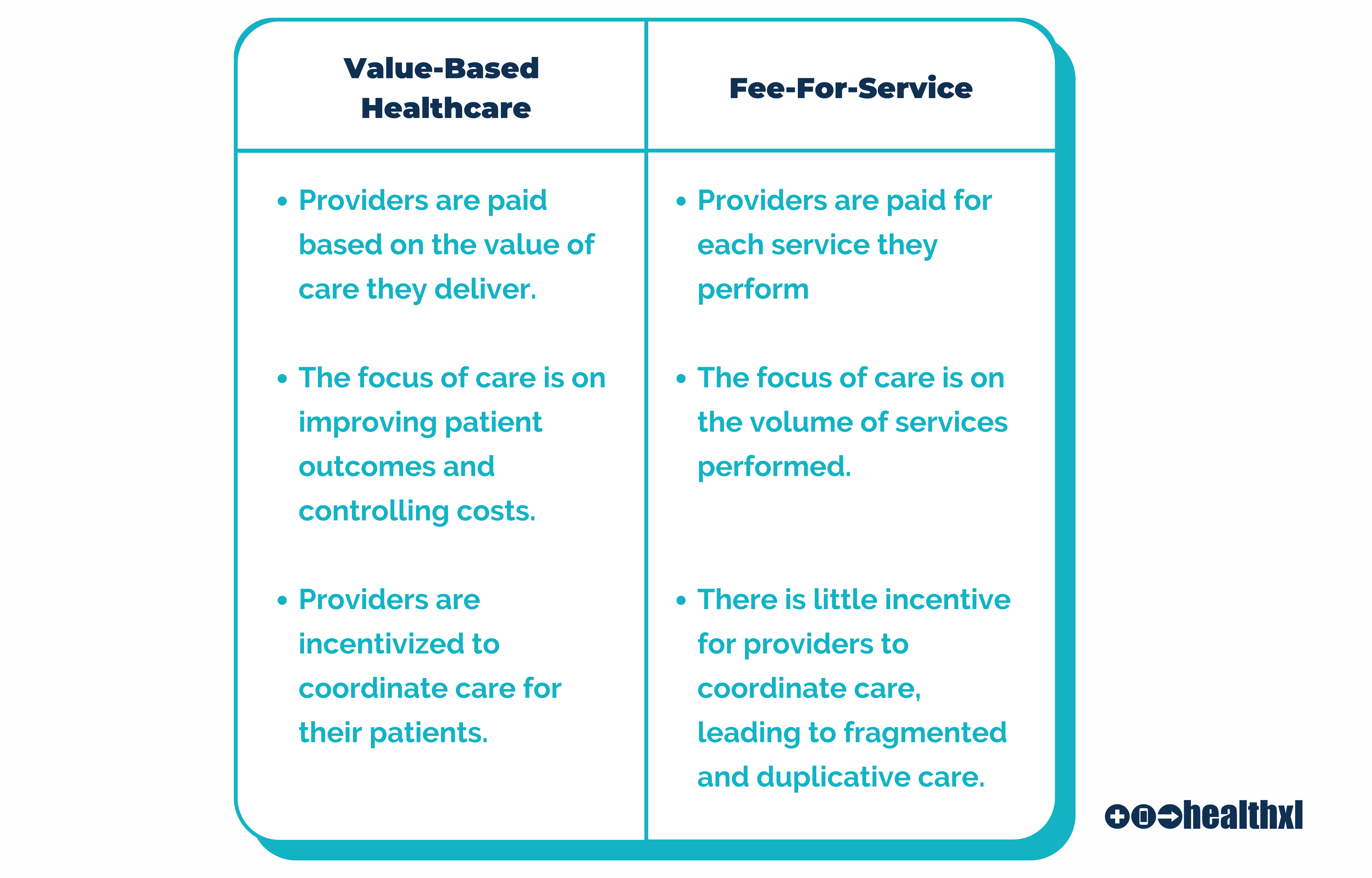
Value-Based Healthcare vs. Fee-for-Service Models
Why is Value-Based Healthcare Important
Value-based healthcare is important because it focuses on improving patient outcomes, controlling costs, encouraging collaboration, empowering patients, and driving innovation in the delivery of care. This results in a more sustainable, efficient, and effective healthcare system that provides high-quality care to patients.
Reimbursement Models for Value-Based Care
There are several reimbursement models for value-based care:
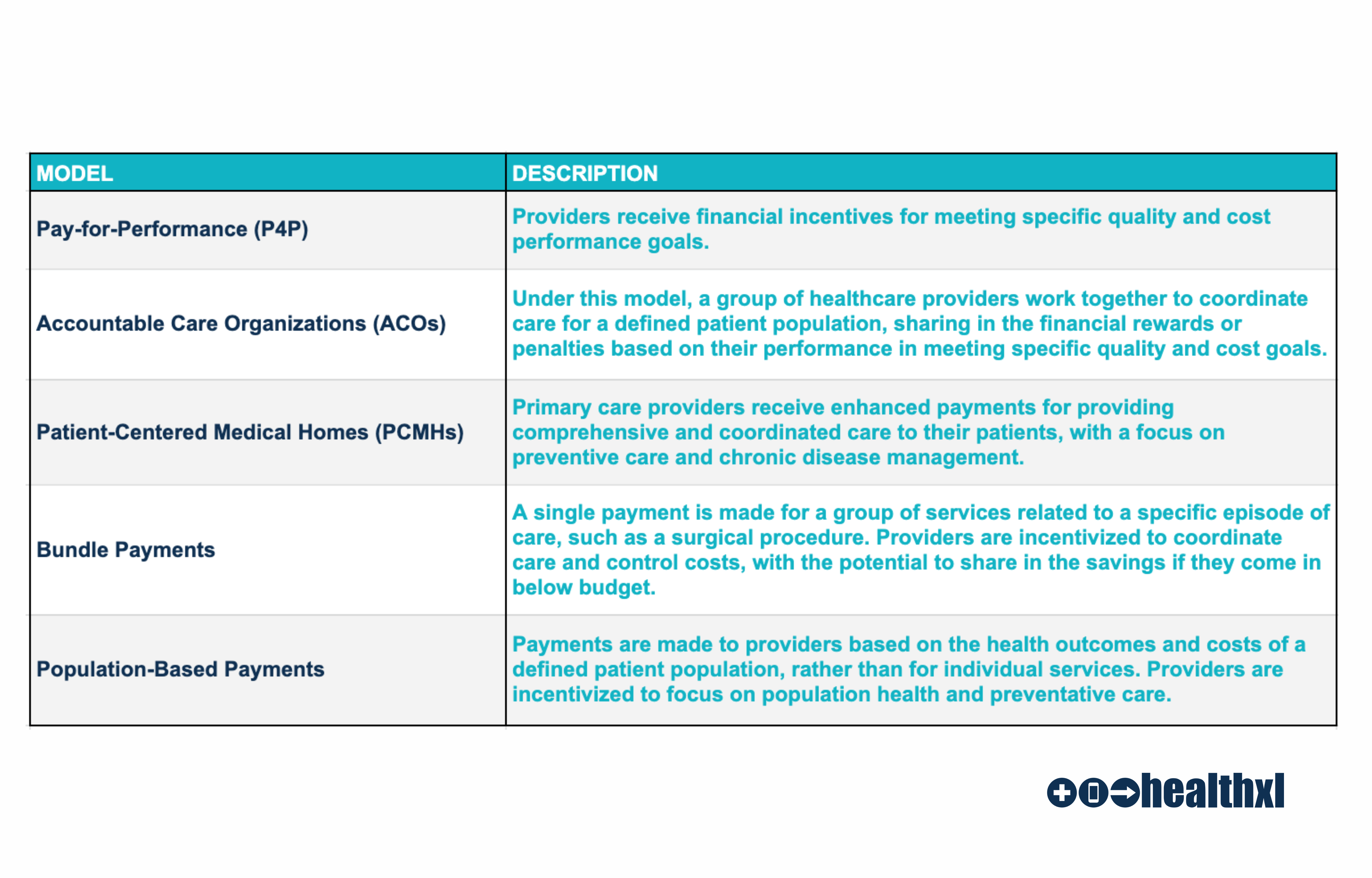
These reimbursement models provide different incentives for providers to focus on improving patient outcomes and controlling costs, and healthcare organizations may choose to use a combination of models to achieve their goals. The choice of reimbursement model will depend on factors such as the patient population, the type of care being delivered, and the goals of the healthcare organization.
Transitioning from Fee-Based to Value-Based Healthcare
The transition from fee-for-service (FFS) to value-based healthcare involves several key steps, including:
Assessment: The first step in transitioning to value-based healthcare is to assess the current healthcare system and identify areas for improvement. This may include evaluating the quality of care, patient outcomes, and cost structure.
Stakeholder engagement: Engaging key stakeholders, including patients, providers, payers, and healthcare organizations, is essential to successfully transition to value-based healthcare. This may involve educating stakeholders on the benefits of value-based care, addressing any concerns they may have, and obtaining buy-in for the transition.
Data and technology: Implementing robust data systems and technologies is essential for tracking and measuring the success of value-based care. This may include electronic health records (EHRs), health information exchanges (HIEs), and population health management tools.
Care redesign: The delivery of care must be redesigned to align with the principles of value-based healthcare. This may involve adopting care models such as patient-centered medical homes (PCMHs) or accountable care organizations (ACOs), or implementing new care processes and protocols.
Reimbursement models: Healthcare organizations must adopt reimbursement models that incentivize value-based care, such as pay-for-performance (P4P) or bundled payments. This may involve negotiating new contracts with payers, or restructuring existing reimbursement arrangements.
Measurement and evaluation: It is essential to continuously measure and evaluate the success of value-based care, using data and metrics to track changes in quality, patient outcomes, and cost. This may involve implementing new performance measures, or adapting existing ones, to reflect the goals of value-based care.
Continuous improvement: The transition to value-based care is an ongoing process, and healthcare organizations must continually seek opportunities to improve and optimize their care delivery processes. This may involve adopting new technologies, adjusting care processes, or adjusting reimbursement models as needed.
Transitioning from fee-for-service to value-based healthcare requires a comprehensive and collaborative effort, involving stakeholders from across the healthcare system. Successful transition requires a commitment to continuous improvement and the adoption of new care delivery models, technologies, and reimbursement models.
To learn about ‘DTx Reimbursement in the US - Value-Based Contracting Basics’, read our Meeting Notes.
Want us to cover a specific topic or explain a new technology or innovation? Write to us at [email protected].


